All published articles of this journal are available on ScienceDirect.
Depression and Anxiety in Pathways of Medically Assisted Reproduction: The Role of Infertility Stress Dimensions
Abstract
Background:
Depressive and anxious symptoms are common psychological reactions to infertility and Medically Assisted Reproduction (MAR). No study compared depressive and anxious symptoms and infertility stress dimensions across homologous and heterologous MAR, nor explored the specific role of the infertility stress dimensions in the two pathways. Homologous MAR may be associated with higher distress as the couple feel that the responsibility to reproduce and carry on the family line falls on them, and they feel inadequate if they are unable to bear children.
Objective:
We compared depressive/anxious symptoms and infertility stress dimensions between individuals undergoing homologous and heterologous MAR. We also explored the association between the infertility stress dimensions and depressive/anxious symptoms separately in two MAR pathways.
Methods:
Two-hundred twenty-six individuals participated [mean age = 39.71 years; 54.45% women]: 118 (52.2%) in homologous and 108 (47.8%) in heterologous MAR. The Fertility Problem Inventory, Beck Depression Inventory-II, and State and Trait Anxiety Inventory-Y form were administered.
Results:
Individuals in homologous MAR had higher depressive/state-trait anxious symptoms, general infertility stress, and infertility-related sexual concerns than those in heterologous MAR. In homologous MAR, social and sexual concerns were associated with depressive/trait anxious symptoms while gender had no effect. In heterologous MAR, male gender was associated with lower state anxious symptoms while infertility stress dimensions had no effect.
Conclusion:
Individuals in homologous MAR are a more distressed subgroup which requires a tailored supportive psychological intervention specifically on sexual and social concerns.
1. INTRODUCTION
Infertility, the failure to achieve a natural pregnancy after 12 months or more of regular unprotected sexual intercourse, is a condition with a severe impact on personal and social identity [1]. Currently, it affects about 10-15% of the couples aged 20 to 44 in Western countries [2]. During the last decade, there has been a significant increase in the access to pathways of Medically Assisted Reproduction (MAR) [3]. Such treatments often involve physical side effects and changes in the couple’s lifestyle [4]. The modern technological advancements and changes in the socio-cultural views on reproductive rights lead to the development of alternative pathways for infertile individuals, such as homologous and heterologous MAR. The first type of pathway is based on an in-vitro fertilization, which uses the couple’s own gametes; heterologous MAR consists of in-vitro fertilization and the involvement of one or more individuals outside the couple (e.g., donation, donation of male gametes, embryo donation, and gestational carrier).
Unmet parenthood expectations due to infertility can produce overwhelming feelings of grief, threat, anger, guilt, and shame. On the other hand, a MAR pathway is often experienced with a perceived lack of control, ambivalent feelings between hope/optimism and a sense of uncertainty/worry about the negative outcome [5].
The assessment of depressive and anxious symptoms in couples undergoing MAR is an important area in the management of infertile couples since those reporting these psychopathological features prior to infertility treatment likely have less physical, emotional, and social resources to cope with the stress of this treatment [6]. Systematic reviews indicated that depressive and anxious symptoms are the most frequent psychological reactions to infertility and start of a MAR pathway [7]. However, a recent systematic review showed inconsistent evidence regarding differences in the levels of these symptoms as compared with the individuals who conceive naturally or normative samples of the general population [8].
It is important to understand the factors associated with psychopathological features to plan effective management strategies. One of the factors which may explain inconsistency in data is gender. For example, clinical depression is prevalent in 26.2% of women and 9.2% of men undergoing MAR, while clinical anxiety is present in 14.8% of women and 4.9% of men [9]. According to a review [10], gender differences moderate the levels of depression and anxiety in infertile couples undergoing MAR, with women reporting higher depression, anxiety, stigma, and shame, although there are no gender differences in the domains of marital adjustment, marital satisfaction, and sexual satisfaction.
Another factor potentially affecting the intensity of depressive and anxious symptoms is infertility stress. In general, stress can be defined as the subjective experience consequent to interpreting an event as threatening to the self and appraising the personal resources as insufficient to cope with it [11]. According to Newton et al. [12], infertility stress includes specific domains such as social, relational, and sexual concerns, unmet needs for parenthood and rejection of a lifestyle without children. Among such stress dimensions, sexual and social concerns were found to be the strongest predictors of infertile individuals’ emotional distress [12].
While the evidence showed a close relationship between infertility stress and depressive/anxious symptoms [13], there is little knowledge about the different roles of the specific infertility stress dimensions across MAR pathways. No study compared depressive/anxious symptoms and infertility stress dimensions across homologous and heterologous MAR, nor explored the specific role of these dimensions in the two pathways. The present exploratory study aimed at comparing the levels of depressive/anxious symptoms and infertility stress dimensions between individuals undergoing homologous and heterologous pathways. We hypothesized that depressive/ anxious symptoms and infertility stress may be higher in homologous MAR than in the heterologous MAR: the couple in homologous MAR might feel that the responsibility falls on them to reproduce and thereby carry on the family line, and they feel inadequate if they are unable to bear children [14]. We also explored specific infertility stress dimensions associated with depressive/anxious symptoms separately in individuals undergoing homologous and heterologous MAR. We hypothesized that the infertility stress dimensions may be more closely associated with emotional distress in homologous MAR than in the heterologous MAR . We also expected that female gender is linked with higher distress in both the pathways since most of the studies found females to be more distressed than males.
2. METHODS
2.1. Inclusion Criteria and Procedure
The study was approved by the Institutional Ethics Committee of the Careggi University Hospital of Florence (Italy) and it was reported in accordance with the ethical standards of the Helsinki Declaration of 1975, as revised in 2008. Participants undergoing a homologous or heterologous MAR pathway at the Medically Prescribed Reproduction unit were invited to participate in the study. Inclusion criteria were: (a) age ≥18 years, (b) good competence in reading/under- standing written/oral Italian language, (c) provision of signed written informed consent. Materials containing personal information about participants were kept on electronic supports protected by passwords.
2.2. Measures
The Fertility Problem Inventory [FPI; 12] is a 46-item questionnaire, which assesses the intensity of the stress related to the various dimensions of infertility on a 6-point Likert scale, with higher scores reflecting severe infertility stress. The measure was developed after a specific process where relevant themes of infertility-related stress were identified by a preliminary examination of the popular and scientific literature. The validation study was conducted on a large sample of infertile women and men who were consecutively referred for assessment and treatment with in-vitro fertilization [12]. A preliminary version including 84 items and seven subscales was created which was further refined for improving content validity and clarity of the items leading to the final version which contains the following five subscales: FPI-Rejection of Childfree Lifestyle (negative view of childfree lifestyle or status quo, future satisfaction or happiness dependent on having a child or another child), FPI-Need for Parenthood (close identification with the role of parent, parenthood perceived as a primary or an essential goal in life), FPI-Sexual Concern (diminished sexual enjoyment or sexual self-esteem, difficulty in sexual relations), FPI-Social Concerns (sensitivity to comments, reminders of infertility, feelings of social isolation, alienation from family or peers), FPI-Relationship Concern (difficulty in talking about infertility, understanding/ accepting sex differences, concerns about the impact on relationship), and FPI-Global Stress (Total score measuring overall infertility-related stress). In the present study, internal consistency was good or excellent in all of the scales; Cronbach’s alpha values: FPI-Rejection of Childfree Lifestyle = 0.81; FPI-Need for Parenthood = 0.88; FPI-Sexual Concern = 0.86; FPI-Social Concerns = 0.90; FPI-Relationship Concerns = 0.82; FPI-Global Stress = 0.91).
The Beck Depression Inventory-II [BDI-II; 15] is a 21-Item questionnaire, which assesses the intensity of the cognitive, affective, and somatic depressive symptoms experienced by the individual during the past two weeks. Higher scores indicate more intense depressive symptoms. In the present study, internal consistency was good (Cronbach’s alpha = 0.84).
The State and Trait Anxiety Inventory-Y form [STAI-Y; 16] is a self-report questionnaire measuring anxiety through a state anxiety scale (STAI-Y State) and a trait anxiety scale (STAI-Y Trait), both containing twenty items on a 4-point Likert scale, with higher scores denoting more intense state/trait anxiety. Internal consistency was good for both the STAI-Y State (alpha = 0.83) and the STAI-Y Trait (alpha = 0.87).
2.3. Data Analysis
Differences between MAR pathways were explored through independent-sample Student t tests. Pearson’s bivariate correlations were calculated between the FPI, BDI-II and STAI-Y scores for homologous and heterologous MAR groups, separately. Correlation values were interpreted as follows [17]: 0 < r < |0.30| = weak; |0.30| < r < |0.50| = moderate; |0.50| < r < |0.70| = strong; |0.70| < r < |1| = very strong. Multivariate analyses of variance (MANCOVAs) were performed on BDI-II and STAI-Y scores and the FPI subscale scores and gender separately for the two groups. Effect sizes were computed as partial squared Eta (η2): values of 0.01, 0.06, and 0.14 were interpreted as small, medium, and large, respectively [18]. Significance was set at p < 0.05. Analyses were performed through the software SPSS version 22.00.
3. RESULTS
3.1. Participants’ Descriptive Characteristics
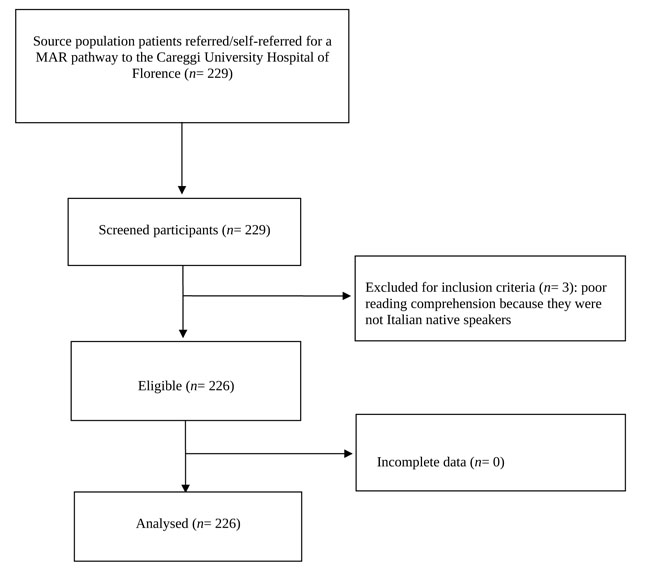
Two hundred and twenty-six participants undergoing a MAR pathway were included [123 females (54.45%); mean age = 39.71, SD= 5.51] (Table 1). Of those, 118 (52.2%) were undergoing homologous and 108 (47.8%) heterologous MAR, respectively. The participants’ flow is presented in Fig. (1) according to the STROBE flowchart [19].
3.2. Comparison of Depressive/anxious Symptoms and Infertility Stress Across Pathways
Thirteen percent, 8.20% and 9.60% of the sample reported clinically significant state and trait anxious and depressive symptoms, as suggested by a score higher than the 90th percentile on the scales. Participants in homologous MAR had significantly higher BDI-II, STAI-Y State, STAI-Y Trait, FPI-Need for Parenthood, and FPI-Global Stress scores than those in the heterologous group (Table 2). A difference was also observed on the FPI-Relationship Concern scores, despite at a borderline significance level.
3.3. Association between Depressive/anxious Symptoms and Infertility Stress Dimensions
In both the homologous and heterologous MAR, scores on the FPI-Sexual Concern, FPI-Social Concern, FPI-Relationship Concern, and FPI-Global Stress correlated moderately with scores on the STAI-Y State, STAI-Y Trait, and BDI-II (Table 3). In homologous MAR, scores on the FPI-Need for Parenthood correlated weakly with scores on the STAI-Y State, STAI-Y Trait, and BDI-II; on the other hand, in heterologous MAR, scores on the FPI-Need for Parenthood correlated moderately with scores on the STAI-Y State, STAI-Y Trait, and BDI-II. In both the pathways, scores on the FPI-Rejection of a Childfree Lifestyle correlated weakly with scores on the clinical scales. The association between socio-demographics (age, number of children, duration of the relationship, duration of seeking pregnancy) and the clinical scale scores were weak in both the groups.
3.4. Role of Infertility Stress Dimensions on Depressive/anxious Symptoms in the Pathways
The results of the MANCOVAs showed that in homologous MAR, infertility-related social and sexual concerns were associated with depressive/trait anxious symptoms and sexual concerns were also related to state anxious symptoms. Infertility stress dimensions and gender had no significant effects. In heterologous MAR, none of the infertility stress dimensions were associated with depressive and state/trait anxious symptoms while only male gender was associated with lower state anxious symptoms. The MANCOVAs are displayed in Table 4.
| - | n / Mean ± SD | % / Range | |
|---|---|---|---|
| Gender | Males | 103 | 45.6 |
| Females | 123 | 54.4 | |
| Age (years) | 39.71 ± 5.51 | 26 – 57 | |
| Marital status | Married | 140 | 61.9 |
| Cohabitant | 86 | 38.1 | |
| Education title | Mid-school license | 27 | 11.9 |
| High-school license | 116 | 51.3 | |
| Degree | 83 | 36.7 | |
| Employment status | Unemployed | 12 | 5.3 |
| Employed | 214 | 94.7 | |
| MAR pathway | Homologous | 118 | 52.2 |
| Heterologous | 108 | 47.8 | |
| Duration of the relationship (months) | 119.29 ±60.75 | 23 – 305 | |
| Duration of pregnancy seeking (months) | 46.48 ±29.68 | 6 – 180 | |
| Clinical scales | MAR Pathway | n | Mean | SD | t(df) | p |
|---|---|---|---|---|---|---|
| BDI-II | Homologous | 118 | 8.83 | 7.20 | 3.75(224) | < 0.001 |
| Heterologous | 108 | 5.32 | 6.81 | |||
| STAI-Y State | Homologous | 118 | 42.77 | 12.28 | 4.52(220.19) | < 0.001 |
| Heterologous | 108 | 36.10 | 9.83 | |||
| STAI-Y Trait | Homologous | 118 | 39.74 | 9.91 | 3.09(224) | 0.002 |
| Heterologous | 108 | 35.82 | 9.01 | |||
| FPI-Rejection of childfree lifestyle | Homologous | 118 | 31.18 | 8.12 | 0.60(224) | 0.54 |
| Heterologous | 108 | 30.56 | 7.03 | |||
| FPI-Need for Parenthood | Homologous | 118 | 37.46 | 10.21 | 1.02(224) | 0.30 |
| Heterologous | 108 | 36.13 | 8.98 | |||
| FPI-Sexual Concern | Homologous | 118 | 17.97 | 7.74 | 2.96(224) | 0.003 |
| Heterologous | 108 | 15.06 | 6.90 | |||
| FPI-Social Concerns | Homologous | 118 | 23.93 | 9.73 | 1.80(224) | 0.07 |
| Heterologous | 108 | 21.70 | 8.66 | |||
| FPI-Relationship Concern | Homologous | 118 | 23.22 | 8.22 | 1.89(224) | 0.05 |
| Heterologous | 108 | 21.18 | 7.85 | |||
| FPI-Global Stress | Homologous | 118 | 133.76 | 30.73 | 2.31(224) | 0.02 |
| Heterologous | 108 | 124.62 | 28.18 |
| 1. | 2. | 3. | 4. | 5. | 6. | 7. | 8. | 9. | 10. | 11. | 12. | 13. | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1.STAI-Y State | 1 | ,697** | ,723** | ,198* | ,163 | ,428** | ,399** | ,330** | ,429** | -,095 | -,049 | ,042 | -,004 |
| 2.STAI-Y Trait | ,799** | 1 | ,741** | ,124 | ,160 | ,472** | ,483** | ,325** | ,445** | -,040 | ,000 | -,025 | -,061 |
| 3.BDI-II | ,756** | ,716** | 1 | ,085 | ,128 | ,496** | ,466** | ,417** | ,449** | -,151 | ,129 | -,016 | -,056 |
| 4.FPI-Rejection of childfree lifestyle | ,223* | ,221* | ,205* | 1 | ,546** | ,141 | ,280** | ,261** | ,640** | -,160 | -,123 | ,211* | ,077 |
| 5.FPI-Need for Parenthood | ,387** | ,363** | ,367** | ,530** | 1 | ,269** | ,290** | ,206* | ,691** | -,156 | -,217* | ,207* | ,142 |
| 6.FPI-Sexual Concern | ,492** | ,453** | ,453** | ,310** | ,515** | 1 | ,540** | ,497** | ,683** | ,059 | ,091 | ,021 | -,112 |
| 7.FPI-Social Concern | ,398** | ,396** | ,335** | ,155 | ,252** | ,542** | 1 | ,530** | ,765** | -,099 | -,025 | -,057 | -,062 |
| 8.FPI-Relationship Concern | ,275** | ,283** | ,294** | ,172 | ,345** | ,537** | ,511** | 1 | ,698** | -,023 | ,051 | -,046 | -,089 |
| 9.FPI-Global Stress | ,498** | ,483** | ,464** | ,590** | ,751** | ,803** | ,702** | ,720** | 1 | -,117 | -,076 | ,100 | -,004 |
| 10.Age | -,145 | -,101 | -,187 | ,003 | ,093 | ,059 | -,114 | ,084 | ,033 | 1 | -,022 | ,132 | ,204* |
| 11.Number of born children | -,125 | ,001 | -,009 | -,019 | -,097 | -,104 | -,015 | -,095 | -,092 | -,042 | 1 | -,106 | -,098 |
| 12.Duration of the relationship (years) |
,122 | ,081 | ,179 | ,013 | ,186 | ,089 | -,030 | ,172 | ,123 | -,042 | -,336** | 1 | ,476** |
| 13.Duration of pregnancy seeking (years) | ,018 | ,036 | ,165 | ,027 | ,106 | -,012 | -,034 | ,066 | ,046 | ,094 | -,038 | ,351** | 1 |
| Homologous MAR Pathways (n = 118) | |||||||
|---|---|---|---|---|---|---|---|
| Outcomes | Parameters | β | t | p | 95% CI |
Partial η2 |
|
| Lower | Upper | ||||||
| BDI-II | Intercept | -,814 | -,296 | ,768 | -6,269 | 4,641 | ,001 |
| FPI-Rejection of a Childfree Lifestyle |
-,037 | -,438 | ,663 | -,206 | ,131 | ,002 | |
| FPI-Need for Parenthood |
-,026 | -,385 | ,701 | -,160 | ,108 | ,001 | |
| FPI-Sexual Concerns |
,277 | 3,014 | ,003 | ,095 | ,458 | ,076 | |
| FPI-Social Concerns |
,164 | 2,157 | ,033 | ,013 | ,314 | ,040 | |
| FPI-Relationship Concerns |
,150 | 1,742 | ,084 | -,021 | ,320 | ,027 | |
| Male gender | -1,286 | -1,111 | ,269 | -3,580 | 1,007 | ,011 | |
| Female gender | 0a | 0a | 0a | 0a | 0a | 0a | |
| STAI-Y Trait | Intercept | 25,350 | 6,543 | ,000 | 17,672 | 33,028 | ,278 |
| FPI-Rejection of a Childfree Lifestyle | -,006 | -,047 | ,962 | -,243 | ,232 | ,000 | |
| FPI-Need for Parenthood | -,012 | -,128 | ,899 | -,201 | ,177 | ,000 | |
| FPI-Sexual Concerns | ,380 | 2,940 | ,004 | ,124 | ,636 | ,072 | |
| FPI-Social Concerns | ,329 | 3,083 | ,003 | ,118 | ,541 | ,079 | |
| FPI-Relationship Concerns | ,012 | ,098 | ,922 | -,228 | ,251 | ,000 | |
| Male gender | ,073 | ,045 | ,964 | -3,155 | 3,301 | ,000 | |
| Female gender | 0a | 0a | 0a | 0a | 0a | 0a | |
| STAI-Y State | Intercept | 24,892 | 5,018 | ,000 | 15,063 | 34,722 | ,185 |
| FPI-Rejection of a Childfree Lifestyle | ,187 | 1,217 | ,226 | -,117 | ,490 | ,013 | |
| FPI-Need for Parenthood | -,067 | -,551 | ,583 | -,309 | ,175 | ,003 | |
| FPI-Sexual Concerns | ,447 | 2,703 | ,008 | ,119 | ,775 | ,062 | |
| FPI-Social Concerns | ,206 | 1,504 | ,136 | -,065 | ,477 | ,020 | |
| FPI-Relationship Concerns | ,125 | ,809 | ,420 | -,181 | ,432 | ,006 | |
| Male gender | -2,855 | -1,369 | ,174 | -6,987 | 1,277 | ,017 | |
| Female gender | 0a | 0a | 0a | 0a | 0a | 0a | |
| Heterologous MAR pathway (n = 108) | |||||||
| Outcomes | Parameters | β | t | p | 95% CI |
Partial η2 |
|
| Lower | Upper | ||||||
| BDI-II | Intercept | -4,951 | -1,540 | ,127 | -11,33 | 1,430 | ,023 |
| FPI-Rejection of a Childfree Lifestyle | ,002 | ,023 | ,982 | -,194 | ,199 | ,000 | |
| FPI-Need for Parenthood | ,136 | 1,572 | ,119 | -,036 | ,308 | ,024 | |
| FPI-Sexual Concerns | ,235 | 1,924 | ,057 | -,007 | ,477 | ,036 | |
| FPI-Social Concerns | ,093 | 1,089 | ,279 | -,077 | ,263 | ,012 | |
| FPI-Relationship Concerns | ,038 | ,402 | ,689 | -,151 | ,228 | ,002 | |
| Male gender | -2,162 | -1,768 | ,080 | -4,588 | ,264 | ,031 | |
| Female gender | 0a | 0a | 0a | 0a | 0a | 0a | |
| STAI-Y Trait | Intercept | 20,023 | 4,712 | ,001 | 11,591 | 28,455 | ,183 |
| FPI-Rejection of a Childfree Lifestyle | ,029 | ,220 | ,826 | -,231 | ,288 | ,000 | |
| FPI-Need for Parenthood | ,175 | 1,534 | ,128 | -,051 | ,402 | ,023 | |
| FPI-Sexual Concerns | ,304 | 1,884 | ,063 | -,016 | ,624 | ,035 | |
| FPI-Social Concerns | ,235 | 2,081 | ,040 | ,011 | ,459 | ,042 | |
| FPI-Relationship Concerns | -,023 | -,186 | ,853 | -,274 | ,227 | ,000 | |
| Male gender | -1,010 | -,625 | ,533 | -4,217 | 2,196 | ,004 | |
| Female gender | 0a | 0a | 0a | 0a | 0a | 0a | |
| STAI-Y State | Intercept | 20,927 | 4,759 | ,000 | 12,201 | 29,652 | ,186 |
| FPI-Rejection of a Childfree Lifestyle | ,012 | ,092 | ,927 | -,256 | ,281 | ,000 | |
| FPI-Need for Parenthood | ,203 | 1,715 | ,090 | -,032 | ,438 | ,029 | |
| FPI-Sexual Concerns | ,354 | 2,120 | ,037 | ,023 | ,685 | ,043 | |
| FPI-Social Concerns | ,226 | 1,932 | ,056 | -,006 | ,458 | ,036 | |
| FPI-Relationship Concerns | -,029 | -,226 | ,822 | -,289 | ,230 | ,001 | |
| Male gender | -4,615 | -2,760 | ,007 | -7,933 | -1,297 | ,071 | |
| Female gender | 0a | 0a | 0a | 0a | 0a | 0a | |
4. DISCUSSION
The present study was the first one in the literature comparing depressive/anxious symptoms and infertility stress dimensions across homologous and heterologous MAR, and exploring the specific role of the infertility stress dimensions in emotional distress associated with the two pathways. Based on previous findings [20], it was hypothesized that homologous MAR is associated with higher emotional distress as the couple feels that the responsibility to reproduce and carry on the family line falls on them, therefore they feel inadequate if they are unable to bear children.
About 10% of the sample experienced clinically significant depressive/anxious symptoms and this result was consistent with previous findings in infertile couples showing that clinical depression and anxiety are common manifestations in infertile couples [21]. It is interesting to note, however, that as a whole the not the subjects were more depressed or anxious than the general population. This result is however in line with evidence from a review showing some inconsistency regarding the differences in depressive/anxious symptoms between infertile individuals and those of the general population [8].
Individuals in homologous MAR had higher depressive/ state-trait anxious symptoms, general infertility stress, and specific infertility-related sexual concerns than the hetero- logous group. Given the link between responsibility beliefs/ uncertainty intolerance and depressive/anxious symptoms [22, 23], it might be speculated that in homologous MAR, seeking pregnancy may become an obsessive emotional concern which might affect a couple’s self-esteem and identity.Couples might feel themselves responsible for the pregnancy outcome; this may increase their expectations/standards regarding the pregnancy outcome leading them to be more worried than in heterologous MAR where the outcome also depends on others. In addition, the homologous pathway might lead the couple to focus their attention exclusively on pregnancy and overlook other aspects of life: this might predispose them to depressive features such as social withdrawal, reduced physical activity, and loss of interest in other daily activities.
Another result was higher levels of sexual concerns in homologous MAR. This evidence is in line with previous data showing sexual problems as common difficulties among infertile couples [4]. Again, in homologous MAR, the attention focus of the couple on pregnancy might reduce their interest in sexual activity. Alternatively, higher sexual concerns in homologous MAR may be attributed to the hormonal changes produced by the medical treatment [24].
Overall, our findings expand the literature and have some implications for psychological and clinical practice suggesting that the homologous pathway may be a group at higher risk for emotional distress requiring tailored monitoring and supportive intervention on depressive/anxious symptoms and sexual problems. Sexual problems should be carefully evaluated in couples undergoing homologous MAR, furthermore couple-based sexual therapy may be an additional strategy.
Significant differences were not found between the two pathways on infertility stress dimensions including relational and social problems, rejection of a childfree lifestyle and need for parenthood. This suggests that the clinical work may not be different in these areas for the two pathways.
Correlational analyses showed that in both the pathways higher sexual, social and relational concerns and general infertility stress were associated with higher depressive/state-trait anxious symptoms. In homologous MAR, the need for parenthood was weakly associated with depressive and state-trait anxious symptoms, while this association was moderate in heterologous MAR. This may support the idea that other processes apart from the need to become a parent may work. In both the groups, rejection of a childfree lifestyle was weakly associated with distress, suggesting that this domain may not be relevant to couples. Also socio-demographics including age, the number of children, duration of the relationship, and duration of pregnancy seeking were not associated with distress in both the groups.
The MANCOVAs showed that in homologous MAR, higher infertility-related social and sexual concerns were associated with higher depressive/anxious symptoms, while the other stress dimensions and gender had no effects. This result highlights the stigmatizing impact of a homologous MAR pathway on couples’ subjective experience.
The close association between social concerns and depressive symptoms may also be interpreted in light of the fact that depression typically is related to an experience of loss: infertility and a homologous MAR may produce a perceived or real loss of a social role as naturally conceiving parent [20]. In addition, it may be believed that in the homologous MAR, the person experiences infertility/MAR as a disease and feels the expectations by others about their parenthood are unmet. These couples may choose isolation from the external world to avoid the trauma of seeing others achieve what they desire [25]. This result highlights the importance of improving social support to reduce depressive/anxious symptoms. The focus on the couple’s resources might increase emotional support and help the partners to alleviate the infertility distress by shifting their attention from seeking parenthood to couple goals and social relationships.
In the homologous MAR, the effect of social concerns supports the data of Li and colleagues [26] indicating social concerns as the dimension most closely associated with poorer mental health. The effect of sexual concerns on depressive/ anxious symptoms was in line with most of the literature where sexual concerns are predictors of emotional distress and highlight the importance of sexual therapy [26].
The lack of an effect of relational concerns and gender is in contrast with previous data on homologous MAR where relational issues were among the strongest sources of emotional distress, females experienced more stress as they felt that their spouses were unable to understand how infertility affects them and worried that they were drifting apart in their relationship [27]. Previous research found females to be more distressed than males [10]: an explanation for this inconsistency can be due to the fact that most of the studies were conducted on infertility and not on samples undergoing MAR. It is possible that the couple starting a MAR pathway has passed through a reprocessing of the trauma related to infertility .
In the heterologous MAR, none of the infertility stress dimensions were associated with emotional distress. This suggests that perhaps the impact of infertility among the individuals undergoing this pathway may be less distressing. Male gender was associated with state anxious symptoms supporting previous literature which shows that males are less distressed than females because they focus on other aspects of the couple’s life including affective commitment [28]. Apart from infertility stress dimensions, other variables may be linked with emotional distress outcomes in heterologous MAR: for example, future research should explore the role of other variables like the gender of the infertile partner, the causes of infertility and moral/religious beliefs endorsed by the couple.
LIMITATIONS AND FUTURE DIRECTIONS
The cross-sectional design allows us to draw conclusions only about the associations between the variables. Future longitudinal research should evaluate the trajectories of these symptoms over time across the two pathways and the different phases of each pathway. As the temporal course of the symptoms in each patient was not monitored, it might be interesting to track this aspect and also assess the duration of the symptoms since their onset. We speculated that some depression- and anxiety-related psychological processes might explain the depressive, anxious and stress levels in homologous MAR, such as worry, responsibility/uncertainty intolerance, social withdrawal, and selective attention. However, future research should measure these mechanisms in a mediational analysis to support these conclusions more reliably. The higher levels of depressive-anxious and stress symptoms in homologous MAR may alternatively be attributed to medical treatment.
CONCLUSION
In conclusion, the present exploratory study is the first one comparing emotional distress across MAR pathways: individuals in homologous MAR might be a more vulnerable group requiring a tailored supportive intervention targeting depressive/anxious symptoms and specific sexual/ social concerns while gender may have a role in state distress during the heterologous pathway. Targeted interventions should be validated for this high-risk group. Our results expand the literature highlighting specific associations between infertility stress dimensions, gender and emotional distress across homologous and heterologous MAR pathways.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The study was approved by the Institutional Ethics Com-mittee of the Careggi University Hospital of Florence (Italy).
HUMAN AND ANIMAL RIGHTS
No animals were used in this research. All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013.
CONSENT FOR PUBLICATION
All patients were included after institutional permission and consent.
AVAILABILITY OF DATA AND MATERIALS
The data supporting the findings of the article are not publicly available but they are available from the corresponding author on reasonable request.
FUNDING
None.
AUTHORS’ CONTRIBUTION
AP designed the study, conducted the literature searches, conducted the statistical analysis, wrote the paper. DD reviewed the paper, edited the final version of the paper, MEC designed the study, collected the data, reviewed the paper. All the authors approved the final manuscript.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
The authors acknowledge the encouragement and support provided by Dr. Shanta kishore, Former Head of Anaesthesia, Alnahda Hospital, Muscat.


